Payment Posting

Payment posting in medical billing
Payment posting is a crucial element in medical billing and plays a vital role in revenue cycle management. It provides providers with an accurate overview of reimbursement trends and overall financial status. Additionally, it is instrumental in efficiently addressing denials. We guarantee our clients a swift turnaround time through a meticulously defined posting process. Adhering to the best payment posting practices and information security regulations, we ensure compliance with industry standards to meet your business requirements.
Our End-to-End Payment
Posting Process

Verify payment details
Thoroughly confirm all intricate patient details outlined in the Explanation of Benefits (EOB), including billed amounts, adjusted figures, allowed amounts, co-pays, etc.

Patient payments
We record all patient payments, whether made by checks, cash, or credit cards, as co-pays or deductibles for services not covered by the payer.

ERA processing
We electronically receive remittance advice, review and directly post payments. Swiftly categorizing ERAs into paid and unpaid facilitates streamlined accounting.

Posting denials
Recording claim denials and either transferring the balance to patient accounts or resubmitting the claim to secondary insurance companies.

EOB processing
Entering specific claim details into corresponding patient accounts for reconciliation, following client-specific rules.
Why Supra Mediinformatics?
- Patient Balances- We ensure accurate account reconciliation and promptly invoice the patient for any remaining balance.
- Reviewing Denials- We precisely post remittance or Explanation of Benefits (EOBs), enabling the Accounts Receivable (AR) team to address denied claims. This process also aids in identifying payer issues that could affect multiple patients.
- Reviewing Write-offs & Adjustments- We thoroughly examine write-offs and adjustments in accordance with fee schedules and policies to uncover any payment errors.
- Secondary Claims- Our efficient EOB processing, swiftly moving from the primary payer to secondary or tertiary payer, accelerates the overall payment completion for claims.
- Identifying Internal Factors– Examining denial and payment details helps uncover internal factors like prior authorization or coding issues, preventing these issues proactively.
- Data Analysis- Our team analyzes data by consolidating payment details and reasons for denied claims, aiding us in accurate revenue forecasting.
- Reconcile Payments with ERAs/EOBs- Our Payment Posting team reconciles incoming checks, credit card payments, and EFTs with statements from payers, ensuring the security of received funds and maintaining control over potential issues such as misrouted funds or lost checks.

We Help You Streamline Payment Posting By

Proactive Reimbursement
Detecting denials related to medical necessity, non-covered services, unauthorized services, etc., and implementing preventive measures to avoid recurrence.

Billing Precision
Adjusting patient obligations for discrepancies between the allowed amount and the payment received.

Claim Discrepancy
Adjusting for Discrepancies: Writing Off Variance in Submitted vs. Received Claims.

Payment Audits
Performing Regular Payment Audits for Updated Receivables.
Payment Surveillance
Monitoring Payment Trends: Detecting Inconsistencies and Patterns.
Payment Posting Software Experience
Our Latest Blogs

Outsourcing Medical Billing Services: A Strategic Approach to Financial Efficiency in Healthcare
In the intricate realm of healthcare management, the task of medical billing can be both complex and time-consuming. To alleviate the administrative burden and enhance
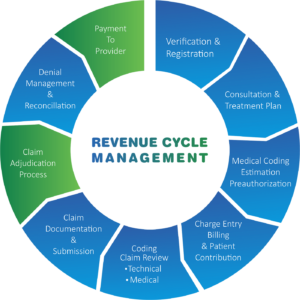
Navigating Financial Success in Healthcare: The Crucial Role of Revenue Cycle Management
In the ever-evolving landscape of healthcare, where patient care takes precedence, the effective management of financial processes is essential for the sustainability and success of

Streamlining Healthcare Finances: The Role of Medical Billing RCM Services
In the complex landscape of healthcare, where the focus is primarily on patient care and well-being, managing the financial aspects efficiently is equally crucial. Medical

Medical Billing Services: When Should It Be Outsourced
Even when many hospitals and medical practices tend to rely upon the expert hands of their in house employees over any other third-party stakeholder, the
Contact Us Today

