Accounts Receivable (AR)

Why is A/R Follow-up Crucial in Medical Billing
Accounts receivable stands as the most substantial and crucial asset for healthcare providers. Our objective is to expedite the recovery of owed funds by consistently identifying and improving processes. We strive to enhance efficiencies at every stage of Healthcare RCM, aligning with industry standards.
Our Detailed Accounts
Receivable Procedure
1
Claims Filing
Submit Claims to the Correct Insurance Provider
2
Tracking Status
Monitor Claims Status with Insurance Provider Follow-up
3
Identifying Denial Causes
Examine and Address Denied Claims by Identifying the Root Cause
4
Following Up Providers
Reach out to Insurance Providers or Patients for Additional Information
5
Refiling Claims
Reprocess the Corrected Claims with the Insurance Carrier
6
Final Payment
Track the Status of Refiled Claims Until Payment is Received
Why Supra Mediinformatics
- Shorten the average AR days to under 45 days
- Decrease AR over 60 days to below 10% of total AR
- Enhance collections to a higher level
- Ensure error-free claims processing
- Optimize collections for faster cash flow
- Cut down administrative costs
- Attain efficiencies beyond in-house billing processes
- Benefit from expert revenue cycle specialists

We Help You Reduce Bad Debt and Improve Cash Flow

Scrutinize all ars
Examine accounts receivable balances, segregate collectible and non-collectible amounts, facilitating the billing of co-insurance/deductible amounts to payers.

Analysis of billing & denials
Outsourcing your accounts receivable services to us ensures a thorough analysis of billing operations, enabling the correction and prevention of issues that may result in claim denials or incorrect payments.

Root cause analysis
Comprehensive examination of accounts to devise an appropriate action plan. Identification and analysis of patterns in codes, procedures, or any operational issues.

Organization’s AR Health
Conduct a comprehensive health check-up of your organization’s A/R aging report by reviewing the provider’s adjustment policy and identifying claims that require immediate adjustments.

Timely filing
Identify claims falling below carrier filing limits and those not paid according to the contract terms. Resubmit all such claims with the required documents.
AR Software Experience
Our Latest Blogs

Outsourcing Medical Billing Services: A Strategic Approach to Financial Efficiency in Healthcare
In the intricate realm of healthcare management, the task of medical billing can be both complex and time-consuming. To alleviate the administrative burden and enhance
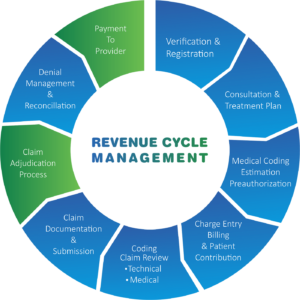
Navigating Financial Success in Healthcare: The Crucial Role of Revenue Cycle Management
In the ever-evolving landscape of healthcare, where patient care takes precedence, the effective management of financial processes is essential for the sustainability and success of

Streamlining Healthcare Finances: The Role of Medical Billing RCM Services
In the complex landscape of healthcare, where the focus is primarily on patient care and well-being, managing the financial aspects efficiently is equally crucial. Medical

Medical Billing Services: When Should It Be Outsourced
Even when many hospitals and medical practices tend to rely upon the expert hands of their in house employees over any other third-party stakeholder, the
Contact Us Today

